TB burden in China
The level of TB in China makes it a major public health problem. China has the world’s second largest TB epidemic after India, with a quarter of the word’s TB burden. In 2014 there were an estimated 930,000 new cases of TB in China, and an estimated 120,000 cases of pulmonary MDR TB. Overall China has 10% of the global burden of TB with 400 million people having latent TB.1
TB control in China
A National Tuberculosis Program was established in 1981 to reform TB control efforts and to expand the reporting system and TB treatment. However, a lack of money hampered the program’s capacity in many areas. This was particularly the case in the poorer provinces with the weakest primary health care infrastructure.2
A nationwide survey in 1990 showed only a slight improvement in TB prevalence compared with rates in 1979 and 1985.
The Chinese Infectious and Endemic Disease Control (IEDC) TB Project

DOTS to stop TB
So in 1991 China launched the 10 year Infectious and Endemic Disease Control (IEDC) project to curb the TB epidemic in 13 of it’s 31 mainland provinces. Part funded by a World Bank loan of $58 million the project adopted the TB DOTS strategy and short course drug treatment which had been developed by the World Health Organisation (WHO) in 1989.3
The project set out to improve the finding of new smear positive cases from 35 percent to 70 percent. It also aimed to increase the cure rate from less than 50% to more than 90% by 2005. If the project could achieve these goals it was estimated that it would save 100,000 deaths every year. It would also cut the TB prevalence by half in those provinces covered by the project.2
Was the IEDC project successful?
The IEDC project was extraordinarily successful with the target of curing 85% of identified patients, achieved within the first two years of the implementation of DOTS. There were not only extremely good cure rates for new TB cases but also for relapsed and re-treatment cases. As a result between 1990 and 2000 the number of people with TB in the DOTS area declined by 36.1%, about 4.1% each year. This compared with a decline of about 4.1 percent in non DOTS areas. However even after seven years the IEDC had only been able to identify about 55% of the TB cases in the project areas.
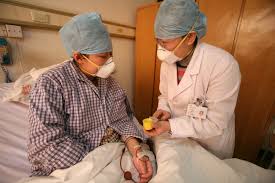
A patient being treated for TB in China © WHO
Also the IEDC project was committed to a free TB service being provided, and it was clear from the start that many provincial and local officials considered a free TB service too expensive. Some considered it unnecessary given China’s cost recovery system for ‘fee for services’. It was clear from the start that senior officials of some project provinces were not prepared to spend significantly increased money, and as a result the project could not reach 100% coverage in all provinces.4
The free TB treatment was in most places also only available to permanent residents. Urban migrants who had relocated from poor rural areas to seek a better life were not eligible for such free services. The predominantly young migrants, numbering more than 150 million, tended to live and work in crowded environments and were unlikely to seek medical care immediately they became ill. This increased the likelihood of them passing on infection.
The project showed that DOTS can be rapidly expanded provided that two critical elements are achieved. Firstly, there is political commitment by government leaders, and secondly a system of TB institutions which allows the rapid dissemination and implementation of a single set of technical guidelines for TB control. Although the use of directly observed therapy was important, other elements of DOTS were equally important.5 The experience with TB control in China had a global impact, as it encouraged the WHO to launch DOTS worldwide.
Political commitment to TB control
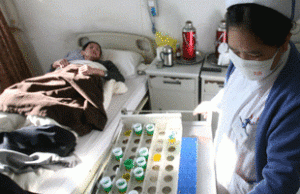
A nurse giving drugs to a patient with MDR-TB
Despite the achievements of the IEDC project there were still problems with the TB control program in China. China still had one of the highest TB burdens in the world. Each year an additional 1.3 million people developed active TB and 150,000 people died. The rate of TB in impoverished rural areas was believed to be nearly three times higher than in the economically developed urban areas.4
Hospitals and clinics continued to function as “for profit” entities, resulting in people who were unable to pay having to abandon their treatment. There were also the issues of Multi-Drug Resistant TB (MDR-TB) and TB/HIV co-infection neither of which were helped by DOTS. Some parts of China had some of the highest rates of MDR-TB in the world.6
Funding for TB
In 2002 the central government increased its funding for TB from US$300,000 per year to $4.8 million per year. Also in 2002 the government arranged a $104 million loan from the World Bank and in the same year they received a $48 million grant from the Global Fund to fight AIDS, TB and Malaria. By late 2002 with increased governmental and international support, DOTS began to expand to all provinces.7 The World Bank funding was used for the China Tuberculosis Control Project, the largest TB control project funded by the World Bank. There was also a smaller project funded by the Department of Health which subsidised treatment for patients in the provinces not covered by the World Bank project.
The China Tuberculosis Control Project 2002 - 2009

Tuberculosis Control Project © World Bank
The TB Control Project covered 16 provinces, selected for their low per capita incomes, high prevalence of TB and a commitment to implementing the program with local financial support. The project would cover the entire populations of the 16 provinces which totaled 688 million in 1999. The project included special measures to benefit vulnerable populations like ethnic minorities, poor women, and older people.4
The project used the WHO DOTS strategy which had been very successfully implemented under the IEDC project. This involved not just finding and curing infectious TB patients, but it also ensured that they received free care as well as taking their full six months of treatment. However, the IEDC project only identified 55% of the TB patients in the project area. So the China Tuberculosis Control Project aimed to have much more extensive and innovative Information, Education & Communication (IEC) programs to raise awareness among the population. It also aimed to reduce the stigma associated with the disease. The programs would involve village committees, women’s groups, traditional health workers and patient support groups among others.
In addition to a free “check and treatment” policy, the project also offered incentives to patients and medical personnel to raise the detection and cure rate. The project also reimbursed patients’ travel expenses between their home and the clinics. Doctors got 20 yuan if the reported a case. They also received 100 to 120 yuan for each patient under their supervision. However the free check and treatment policy only covered diagnosis and first line drugs. Patients still had to pay for drugs that reduced side effects and tests such as liver tests.
From 2002 to 2009, the project treated approximately 1.598 million new smear positive patients. 1.505 million patients completed their treatment (94.2%) and 1.499 (93.8%) million patients were cured. The project achieved a number of other objectives, including reducing the number of TB associated deaths by 770,000.
5th Nationwide TB Prevalence Survey
In 2010 the 5th Nationwide TB Prevalence Survey took place in China. The survey showed that the estimated number of TB patients in the whole population was 5.2 million, giving a prevalence for pulmonary TB of 459 per 100,000. This meant that there had only been a slight decline in prevalence since 2000 when the figure was 466 per 100,000. For smear positive patients however there was a very large decline from 169 per 100,000 in 2000 to 66 per 100,000 in 2010.
China’s case detection rate of new TB cases was 80% and it’s cure rate for new TB cases was above 90%. More than 4.5 million smear positive patients were cured between 2001 and 2010, and China achieved its millennium development goal for TB control five years early.
Drug resistant TB in China

Beijing meeting, with Director General of the WHO Magaret Chan, Bill Gates, and Minister Chen Zhu from China
This didn’t however solve the problem of drug resistant TB in China. The 2000 national TB prevalence survey had shown that one in ten patients with TB had MDR-TB. Other studies confirmed a serious epidemic of MDR TB in several Chinese provinces, with rates of MDR in previously untreated cases that were five to ten times higher than the global average. 8
The National Survey of Drug-Resistant TB in 2007, showed one third of new TB cases and one half of previously treated cases showed some drug resistance. 9
This survey was referred to at the ministerial meeting of high burden M/XDR-TB countries held in Beijing in April 2009. The preliminary findings of the survey were said to show that 8.32% of pulmonary TB patients in China have MDR-TB and 0.68% have XDR-TB. Based on these data it was estimated that there are 120,000 new cases of pulmonary MDR-TB in China each year.10 The actions that the Chinese health authorities were going to take to tackle drug resistant TB were also set out by Minister Chen Zhu.
Current statistics for TB in China
The WHO estimated that in 2015 China had 57,000 cases of multi drug resistant TB.
A total of approximately 900,000 new cases of TB are reported annually, with the highest prevalence of TB in China being in the Xinjiang Uygur automous region with 184.5 people out of 100,000. The incidence of TB in China is expected to be reduced to below 58 per 100,000 people by 2020.
- “Global Tuberculosis Report”, WHO, Global tuberculosis report 2015[↩]
- J Fischer-Mackey, “Controlling Tuberculosis in China, Case Study 3”, 2010, Center for Global Development[↩][↩]
- B Andrews, “Medical Transitions in Twentieth-Century China”, Indiana University Press[↩]
- “Project Appraisal Document on a Proposed Loan in the amount of US$104 million to the People’s Republic of China”, World Bank, 2002, China - Tuberculosis Control Project (English)[↩][↩][↩]
- X Chen, “The DOTS strategy in China: results and lessons after ten years”, Bulletin of the World Health Organisation 2002, 2002, DOTS strategy in China[↩]
- “China: Tuberculosis Control Project”, The World Bank, 2010, China: Tuberculosis Control Project[↩]
- L, Wang, “Progress in tuberculosis control and the evolving public-health system in China”, The Lancet, 2007, Progress in TB control[↩]
- L, Wang “Progress in tuberculosis control and the evolving public health system in China”, The Lancet, 2007, Progress in tuberculosis control[↩]
- Q Long, “Drug-resistant tuberculosis control in China: progress and challenges”, Infect Dis Poverty, 2016, Drug-resistant tuberculosis control[↩]
- “Speech at the Ministerial Meeting of High M/XDR-TB Burden Countries”, 2009, Speech by Minister Chen Zhu[↩]

Would you like to send us a comment about this page?