Tuberculosis continues to be a disease of major importance in South Africa. An estimated 328,000 South Africans became ill with TB in 2020, and an estimated 61,000 people died from TB.1
The very high number of people with HIV in South Africa is increasing the number of people with active Tuberculosis. Of the 61,000 people estimated to have died, an estimated 36,000 were HIV positive. TB continues to be the single largest contributor to death in South Africa. There is more about the relationship between HIV and TB.
As well as being driven by HIV, the TB burden is also driven by poor living conditions and late presentation to health facilities.
The South African government is making major efforts to combat both HIV and TB as set out in its National Strategic Plans (NSPs).
TB in South Africa - National Strategic Plans (NSPs)
National Strategic Plan on HIV, TB and STIs 2017 - 2022
At the launch of this national strategic plan (NSP) the South African Government said:
"We have made major gains in terms of treating millions of people living with HIV & TB, slashing the death toll due to these infections, and reducing the number of new infections. However, there is still a great deal to be done"
The Treatment Action Campaign initially refused to accept the plan.2
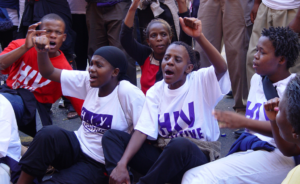
TAC initially refused to accept the latest plan on HIV & TB in South Africa
The overall goal of this NSP is the elimination of HIV, TB and STIs as public health threats by the year 2030. The approach taken in this latest National Strategic Plan is to intensify efforts in the geographic areas that are most affected by TB. In addition the highest impact interventions are to be used in these areas. There is very little mention of drug resistant TB.
The outline of the 2017 NSP is:
Focus for Impact
Comprehensive prevention and care for TB will be provided countrywide but intensified concentrated efforts will be made in the 19 districts with the highest TB burden. In these high burden districts the aim is a saturation of high impact prevention and treatment services.
Highest TB burden
The 19 districts with the highest TB burden in 2015 when the NSP was developed were:
- Gauteng: City of Johannesburg, Ekurhulleni, City of Tshwane, West Rand
- KwaZulu-Natal: eThekwini
- Mpumalanga: Ehlanzeni
- Eastern Cape: Oliver Tambo, Nelson Mandela Metro, Chris Hani, Buffalo City, Saartjie Baartman
- Free State: Mangaung Metro, Lejweleputswa
- North West: Bojanala, Dr Kenneth Kaunda
- Limpopo: Greater Sekhukhune, Waterberg
- Western Cape: City of Cape Town, West Coast
There is more about these districts on the TB Statistics for South Africa page.
Key Populations for TB
The Key Populations for TB are:
- People living with HIV
- Household contacts of TB patients
- Health care workers
- Inmates
- Pregnant women
- Children < 5 years old
- Mine workers and people in peri-mining communities
NSP Mid term NSP report
In December 2019 the Mid-term review was published of the National Strategic Plan for HIV, TB and STIs 2017 - 2022.3
It was found that South Africa has made significant progress towards meeting the 90-90-90 targets set by UNAIDS. But a lot still needs to be done in terms of finding people with TB as well as reducting TB related deaths.
TB in South Africa - Global Plan to End TB 2016 - 2020

Global Plan To End TB
South Africa has also committed to the Global Plan to End TB 2016 - 2020. Set by the Stop TB Partnership this involves implementing the 90-90-90 strategy for TB. Three main targets have been set.
Target 1 is that 90% of all TB cases should be found and given effective treatment.This requires early detection and the prompt treatment of 90% of people with TB. This includes both drug susceptible and drug resistant TB. It also means 90% of people who require preventive therapy. By improving the rates at which people are diagnosed and treated, countries can reduce the spread of TB and reduce incidence.
Target 2 is that as part of this approach 90% of the TB cases in key populations should be found and provided with appropriate treatment.
Target 3 is that there should be a 90% treatment success rate among people identified as needing treatment. This includes treatment for drug susceptible TB, drug resistant TB, or preventive TB therapy. This target is more ambitious than previously established targets for treatment success, as it covers 90% of all people diagnosed with TB, not just those who start treatment.
TB in South Africa - the TB Care Cascade
The focus of the National TB Programme in South Africa has historically been on treatment success rates. This fails to reflect "upstream" losses contributed by individuals who do not access health services. It also fails to reflect those people for whom TB is not diagnosed, notified and treated.
One study of the TB care cascade in South Africa suggests that only just over half (53%) of all TB cases in South Africa in 2013 were successfully treated, with substantial losses during TB diagnosis, linkage to care, and retention in care.4
Some people have suggested that there are also major gaps in the prevention and treatment goals.5 There are also considered by some people to be glaring health system constraints to achieving the goals.
Treatment Action Campaign

Community Health Workers
A report from the Treatment Action Campaign paints a picture of a public healthcare system that is often so severely dysfunctional that it hinders the implementation of HIV and TB programmes. It cites the lack of TB infection control in many clinics and hospitals as an example.
The plan shifts all the responsibility for its implementation to provinces. The principle may be sound, but the NSP provides little guidance to provinces on how to do this or how it will be measured.
Also much of what the plan proposes will require increases in human resources. Community health workers play a vital role in tracing some of those most at risk of TB, including those who have been in close contact with TB patients.
TB in South Africa - drug supplies
Delivering the services outlined in the NSP requires a well functioning supply chain. In a Stop Stockouts National Survey health facilities nation wide reported nearly one in five stock-outs of TB medicines resulted in the patient leaving the health facility without medication.
TB in South Africa - the costs
The total cost of implementing the proposed NSP over the five year period is R207 billion. Mobilisation of additional domestic resources is limited by a number of factors including the country's low economic growth. The NSP hardly makes mention of what proposed interventions may cost or if South Africa has the resources to fund them. As a result many of the NSP's interventions may end up unfunded and thus unimplemented.
Page Updating
This page was last updated in May 2022.
Author Annabel Kanabus
Social Media
If you have found this page useful please tell other people about TBFacts.org and if you have a website please link to us at tbfacts.org/tb-south-africa/
Footnotes
- “Global Tuberculosis Control 2021, WHO, Geneva, 2021, www.who.int/tb/publications/global_report/en/[↩]
- "TAC and section27: We cannot endorse the HIV and TB plan (NSP) in its current form", Section27, 2017, http://section27.org.za/2017/03/tac-and-section27-we-cannot-endorse-the-hiv-and-tb-plan-nsp-in-its-current-form/ [↩]
- sanac.org.za[↩]
- P Naidoo, "The South African Tuberculosis Care Cascade: Estimated Losses and Methodological Challenges", Journal of Infectious Diseases, November 2017, https://academic.oup.com/jid/article/216/suppl_7/S702/4595546[↩]
- "Will the current National Strategic Plan enable South Africa to end AIDS, Tuberculosis and Sexually Transmitted Infections by 2022?", Southern African Journal of HIV Medicine, 2018, https://sajhivmed.org.za/index.php/hivmed/article/view/796 [↩]

Would you like to send us a comment about this page?